
80 percent of heme is generated from the catabolism of RBC, and the remaining 20 percent is generated from ineffective erythropoiesis and breakdown of muscle myoglobin. The body produces 4 mg per kg of bilirubin from the metabolism of heme. To understand the presence of bilirubin in the urine, it is important to understand the physiology behind bilirubin metabolism which can be divided into three phases: prehepatic, hepatic, and posthepatic. Therefore, bilirubinuria is a marker of conjugated hyperbilirubinemia and can be the earliest sign of hepatic or biliary disease. In a healthy individual with normal liver function and bile duct anatomy, bilirubin is not detectable in the urine. Patients may describe their urine as tea or cola-colored when they have jaundice and conjugated hyperbilirubinemia due to liver or biliary disease. 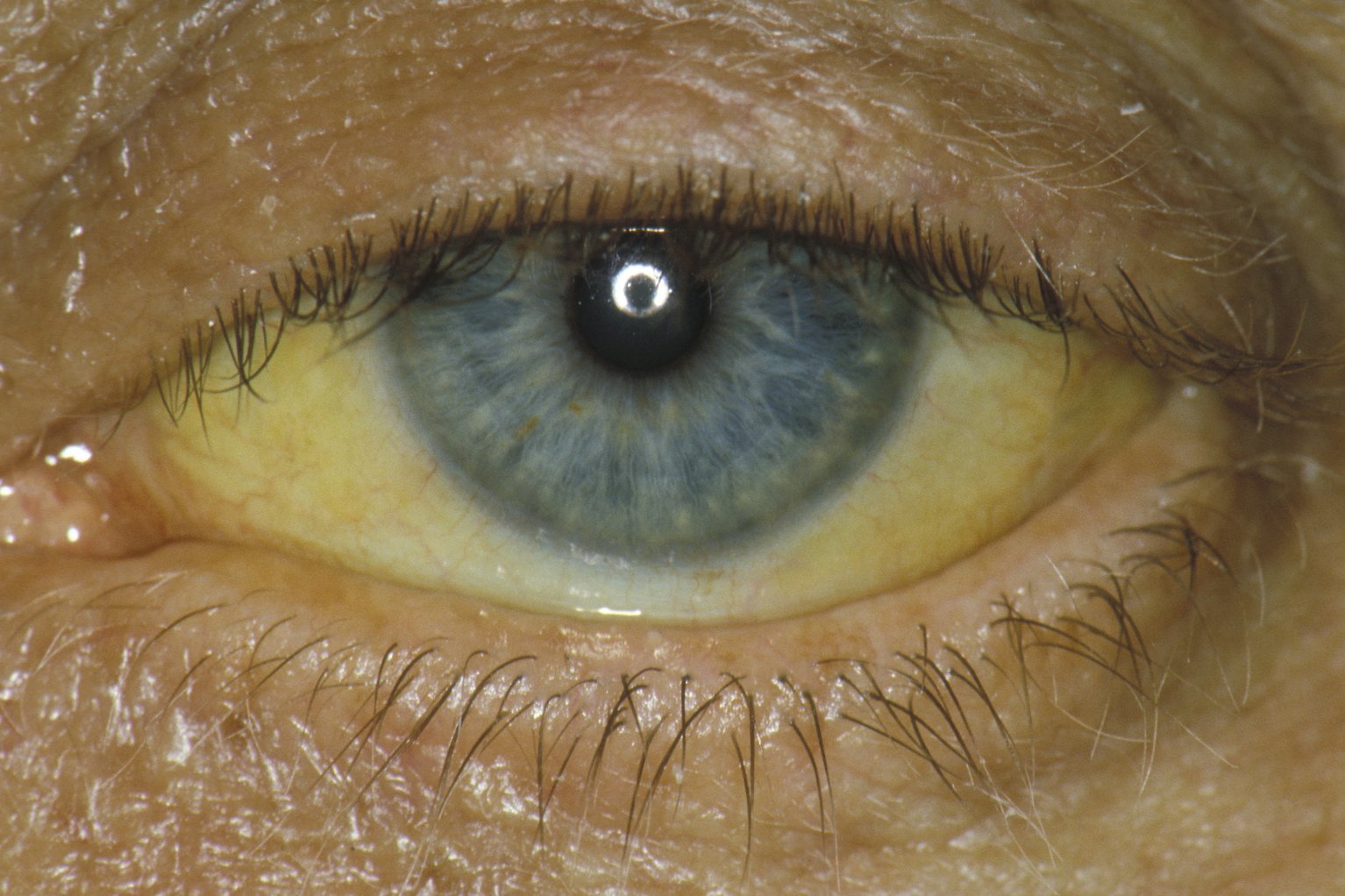
On the other hand, conjugated bilirubin is water-soluble and thus can be renally excreted and detected in the urine. Unconjugated hyperbilirubinemia is characterized by acholuric jaundice as urine is not darkened by urinary bilirubin as bilirubin is not detected in the urine in such cases. Unconjugated bilirubin is soluble in fat but insoluble in water and thus cannot be renally excreted. Bilirubin in the body exists as either conjugated/direct or unconjugated/indirect. Bilirubin and related breakdown metabolites are well known for causing the characteristic coloring in bile and stool however, its presence in the urine is not normal, and for it to be present there, it must be water-soluble and excreted by the kidney. It can be detected by the standardized urine dipstick, mostly referred to as urinalysis in most hospitals worldwide. 1990 99:1396-400.Bilirubinuria is the presence of bilirubin in the urine. A 21-year experience with major hemorrhage after percutaneous liver biopsy. McGill DB, Rakela J, Zinsmeister AR, Ott BJ. A prospective study on the value of ultrasound, computed tomography and endoscopic retrograde cholangiopancreatography in the diagnosis of unjaundiced cholestasis. Pasanen PA, Partanen K, Pikkarainen P, Alhava E, Pirinen A, Janatuinen E. The SGOT/SGPT ratio-an indicator of alcoholic liver disease. Special considerations in interpreting liver function tests. Schramm C, Kanzler S, zum Buschenfelde KH, Galle PR, Lohse AW. Carotenodermia: an erroneous diagnosis of jaundice. Pinto F, Mognol D, Garbelotto G, Dannhauser D, Grava G, Sanzuol F. Diagnosis and therapy of cholestatic liver disease. Extrahepatic manifestations of chronic viral hepatitis. Psychiatric morbidity in patients with alcoholic liver disease. 
1997 11(5 pt 1):406-11.Įwusi-Mensah I, Saunders JB, Wodak AD, Murray RM, Williams R. Vulnerability to psychologic distress and depression in patients with end-stage liver disease due to hepatitis C virus. Singh N, Gayowski T, Wagener MM, Marino IR. Vagaries of clinical presentation of pancreatic and biliary tract cancer. Jaundice in older children and adolescents. In a few instances, more invasive procedures such as cholangiography or liver biopsy may be needed to arrive at a diagnosis. If the complete blood count and initial tests for liver function and infectious hepatitis are unrevealing, the work-up typically proceeds to abdominal imaging by ultrasonography or computed tomographic scanning. The laboratory work-up should begin with a urine test for bilirubin, which indicates that conjugated hyperbilirubinemia is present. Gallstone formation is the most common and benign posthepatic process that causes jaundice however, the differential diagnosis also includes serious conditions such as biliary tract infection, pancreatitis, and malignancies. Posthepatic disorders also can cause conjugated hyperbilirubinemia. The conjugated (direct) bilirubin level is often elevated by alcohol, infectious hepatitis, drug reactions, and autoimmune disorders. Intrahepatic disorders can lead to unconjugated or conjugated hyperbilirubinemia. Prehepatic causes of jaundice include hemolysis and hematoma resorption, which lead to elevated levels of unconjugated (indirect) bilirubin. Organizing the differential diagnosis by prehepatic, intrahepatic, and posthepatic causes may help make the work-up more manageable. Jaundice in an adult patient can be caused by a wide variety of benign or life-threatening disorders.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
